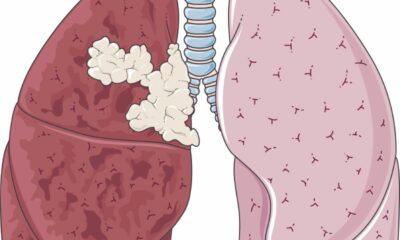
Two genes, NEK2 and INHBA, have been found to be the root of chemotherapy resistance in patients with head and neck cancer. Surprisingly, cancer cells that had previously resisted chemotherapy start to respond when these genes are silenced.
The scientists selected two compounds (Sirodesmin A and Carfilzomib) from a chemical library that can target these genes, making resistant cells significantly more susceptible to the chemotherapeutic medication cisplatin.
This ground-breaking discovery paves the way for more individualised cancer therapy, giving hope to patients who have failed to respond to standard treatments.
Important facts The found genes, NEK2 and INHBA, provide the first proof that head and neck squamous cell cancer (HNSCC) is caused by chemoresistance. Sirodesmin A, a toxin from a fungus, and carfilzomib, a toxin from a bacteria, can both make resistant cells 30 times more vulnerable to chemotherapy. HNSCCs account for more than 90% of head and neck cancer cases, and their 5-year survival rate is around 25%.
The two genes were shown to actively “work” in the majority of human cancer types, suggesting that the discoveries might apply to additional malignancies with high quantities of the genes.
Additionally, the researchers looked through a chemical library, which is frequently used in drug development, and discovered two compounds that might precisely target the two genes and render resistant cancer cells nearly 30 times more susceptible to the chemotherapy treatment cisplatin.
They could be used in conjunction with chemotherapeutic drugs like cisplatin to do this by lowering the levels of the two genes. Sirodesmin A, one of these chemicals, is a fungus toxin, while Carfilzomib, the other, is a bacterial product.
This suggests that rather than needing to research and produce new medications, it may be possible to modify already-available ones to target novel illness causes.
The study, conducted by Queen Mary and published in Molecular Cancer, provides the first proof that the genes NEK2 and INHBA contribute to chemoresistance in head and neck squamous cell carcinoma (HNSCC) and that gene silencing can reverse chemoresistance to a variety of medications.
To find genes that might alter a tumor’s susceptibility to medication therapy, researchers first employed a technique called data mining. They examined 4’significant’ genes that were highly sensitive after testing 28 genes on 12 strains of chemoresistant cancer cell lines. These genes were further examined, and they were evaluated for multidrug resistance.
This means that existing drugs may be modified to target new disease causes rather than having to be researched and created.
The Queen Mary study, which was published in the journal Molecular Cancer, offers the first evidence that the genes NEK2 and INHBA are involved in head and neck squamous cell carcinoma (HNSCC) chemoresistance and that gene silencing can overcome this resistance to a number of drugs.
Researchers first used a method known as data mining to uncover genes that might affect a tumor’s sensitivity to pharmaceutical therapy. After examining 28 genes on 12 different strains of chemoresistant cancer cell lines, they focused on 4 “significant” genes that were very sensitive. Further research was done on these genes, and their potential for multidrug resistance was assessed.
“These results are a promising step towards cancer patients in the future receiving personalised treatment based on their genes and tumour type that gives them a better survival rate and treatment outcome,” said Dr. Muy-Teck Teh, senior author of the study from Queen Mary University of London.
Unfortunately, many people out there do not benefit from chemotherapy or radiation. However, our research has demonstrated that, at least in head and neck malignancies, these two specific genes may be to blame. These genes can subsequently be targeted to combat chemoresistance.
“Treatment that doesn’t work is damaging both for the NHS and patients themselves. There can be costs associated with prolonged treatment and hospital stays, and it’s naturally extremely difficult for people with cancer when their treatment doesn’t have the results they are hoping for.”
HNSCCs account for 90% of all head and neck cancers, with tobacco and alcohol use being the main risk factors. Each year, 12,422 new cases of head and neck cancer are diagnosed, and less than 25% of individuals with advanced HNSCC survive for at least 5 years after diagnosis. HNSCC survival rates are often low due in large part to treatment failure brought on by chemo- and/or radiation resistance.
Contrary to lung and breast cancer patients, all HNSCC patients receive nearly identical treatment regimens regardless of the genetic makeup of their tumour.
Many patients with head and neck squamous cell carcinoma (HNSCC), who require multimodal therapy combining chemotherapy in conjunction with surgery and/or radiotherapy, experience treatment failure due to multidrug resistance. Uncertain molecular processes confer chemoresistance.
Using transcriptome data mining, functional assays against cisplatin, 5-fluorouracil (5FU), paclitaxel (PTX), and docetaxel (DTX) on 12 strains of chemoresistant cell lines were performed on 28 genes.
Ten genes were discovered that confer multidrug chemoresistance (TOP2A, DNMT1, INHBA, CXCL8, NEK2, FOXO6, VIM, FOXM1B, NR3C1, and BIRC5). Four of these (TOP2A, DNMT1, INHBA, and NEK2) were elevated in a population of 221 HNSCC patients. All drug-resistant cell strains lost their chemoresistance when NEK2 was silenced. The majority of the drug-resistant cell strains were found to confer chemoresistance with INHBA and TOP2A, although DNMT1 had variable findings.
Pan-cancer INHBA and NEK2 have substantial predictive significance in at least 16 cancer types, according to a Kaplan-Meier survival analysis of 21 human cancer types. Two substances (Sirodesmin A and Carfilzomib) targeting both INHBA and NEK2 and re-sensitizing cisplatin-resistant cells were found using drug library screenings.
We have shown the first proof that NEK2 and INHBA confer chemoresistance in HNSCC cells, and that silencing either gene using siRNA abolished multidrug chemoresistance. To combat cisplatin chemoresistance in HNSCC, the two currently available drugs might be repurposed.
This discovery could result in brand-new, biomarker-linked treatments that target specific individuals and can prevent or abate chemoresistance in HNSCC and other cancer types with high NEK2 and INHBA expression. To define their signalling mechanisms in cancer chemoresistance, more research is required.
 Diabetology1 week ago
Diabetology1 week ago
 Diabetology5 days ago
Diabetology5 days ago
 Diabetology13 hours ago
Diabetology13 hours ago
 Diabetology13 hours ago
Diabetology13 hours ago