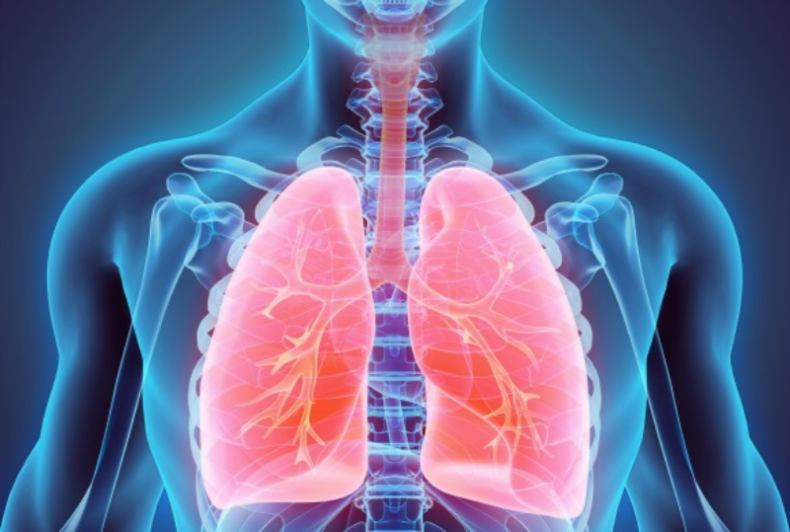
Comprehending the intricate ecosystem of bacteria in the lungs is essential in the fight against the degenerative hereditary disease known as cystic fibrosis (CF), which affects the lungs. Chronic infections are common in CF patients, which can cause inflammation and, eventually, respiratory collapse. The reality of cystic fibrosis (CF), in which several bacteria are present in the lungs at all times, is not well suited to traditional perspectives on infection, which center on a single pathogen producing a single disease. Understanding this intricacy, Northumbria University researchers have started a study to understand the ecological dynamics of lung infections in people with cystic fibrosis.
This latest study followed 30 CF patients, both adults and children, for three years while keeping an eye on their lung microbiota—the population of microbes living in the lungs. The idea was to track changes in these communities over time in order to spot trends that would guide more effective treatment plans. This research is unique in that it applies ecological concepts to explain the lung environment in cystic fibrosis (CF). Specifically, it uses island biogeography, which is the study of species distribution on isolated natural habitats such as islands.
The bacteria the researchers observed were divided into two groups: intermittent colonizers, which come and go, and chronic colonizers, which are continuously present and frequently cause persistent illnesses. They found evidence of the persistence and increased frequency of chronic colonists compared to earlier estimates, which is not fully captured by typical cultural approaches. In the lung ecology, however, intermittent colonizers were rare and signified the passing guests.
The study used Vellend’s concept of ecological processes and species-time linkages to explain how these groups contribute to changes in the lung microbiota over time. It was discovered that the makeup of the chronic group stayed mostly constant, controlled by a process known as homogenizing dispersal, which allows comparable bacteria to proliferate in a variety of lung conditions. The intermittent group, on the other hand, was more erratic due to sporadic events and changes, or drift.
Remarkably, there seems to be a correlation between these ecological processes and the patients’ lung function. greater homogenizing dispersal rates in adults were related with declining lung function, while greater drift rates were linked to improving lung function. This implies that CF patients’ health may be directly impacted by the stability of the microbial flora in their lungs.
The results of the study are consistent with past investigations that have demonstrated the intricacy of interactions among microbial populations in CF lungs. For example, bacterial species can change how they behave with one another, which can occasionally result in a greater resistance to antibiotics. Furthermore, the respiratory tract is constantly being cleaned of bacteria by the lung microbiome, which is very dynamic and can become disturbed in disease conditions. Furthermore, pathogens like Staphylococcus aureus and Pseudomonas aeruginosa, which are frequently detected in greater quantities by molecular techniques like quantitative PCR, may be underreported by classic culture methods. Building on previous discoveries, the Northumbria University study offers a more complex picture of the microbial environment in CF lungs.
There are significant clinical ramifications for this discovery. Healthcare professionals can more effectively target the chronic colonizers that contribute most to the advancement of disease by understanding the ecological patterns and processes at work, while also taking the function of intermittent colonizers into consideration. The study also emphasizes the necessity of developing more advanced diagnostic instruments in order to precisely map the lung microbiota and monitor its changes over time.
Finally, the research from Northumbria University provides a novel insight into the lung infections that afflict individuals with cystic fibrosis. Through the application of ecological theory to medical research, patterns have been found that may lead to more successful treatments, which may ultimately improve the lives of those afflicted with this difficult illness.

 Diabetology2 weeks ago
Diabetology2 weeks ago
 Diabetology2 weeks ago
Diabetology2 weeks ago
 Diabetology1 week ago
Diabetology1 week ago
 Diabetology1 week ago
Diabetology1 week ago
 Diabetology1 week ago
Diabetology1 week ago
 Diabetology2 weeks ago
Diabetology2 weeks ago
 Diabetology1 week ago
Diabetology1 week ago
 Diabetology2 weeks ago
Diabetology2 weeks ago