For people living with diabetes, blood sugar monitoring is a cornerstone of effective management. This vital practice allows you to understand how your body reacts to food, exercise, medications, and other factors that influence blood sugar levels. This article delves into the different types of blood sugar monitoring tools, explains why monitoring is crucial, and provides guidance on interpreting your readings and using them to optimize your diabetes care.
Understanding Blood Sugar (Glucose)
Blood sugar, also known as glucose, is the primary source of energy for your cells. It comes from the carbohydrates you consume, and your body regulates blood sugar levels through the hormone insulin. In people with diabetes, this regulation can be impaired, leading to either chronically high blood sugar (hyperglycemia) or dangerously low blood sugar (hypoglycemia).
The Role of Blood Sugar Monitoring in Diabetes Management
Blood sugar monitoring empowers you to:
- Track Blood Sugar Fluctuations: Gain insights into how your blood sugar levels change throughout the day in response to various factors.
- Evaluate Treatment Effectiveness: Monitor the effectiveness of your diabetes management plan, including medications, diet, and exercise.
- Identify Trends: Identify patterns in your blood sugar levels and adjust your treatment plan accordingly.
- Prevent Complications: Help prevent long-term complications associated with diabetes by maintaining blood sugar within a healthy range.
- Make Informed Decisions: Empower yourself to make informed decisions about diet, exercise, and medication adjustments based on your blood sugar readings.
Types of Blood Sugar Monitoring Systems
There are two main types of blood sugar monitoring systems:
- Self-Monitoring of Blood Glucose (SMBG): This is the traditional method where you use a finger prick to draw a small blood sample and test it using a glucometer.
- Continuous Glucose Monitoring (CGM): These systems utilize a sensor inserted under the skin that measures glucose levels in the interstitial fluid (fluid surrounding cells) every few minutes and transmits data to a receiver or mobile app for real-time monitoring.
Choosing the Right Monitoring System
The right monitoring system depends on your individual needs and preferences. Here’s a breakdown of factors to consider:
- Frequency of Monitoring: People with Type 1 diabetes or those taking insulin may need to monitor more frequently than those with Type 2 diabetes managed by diet and exercise alone.
- Lifestyle Considerations: Consider your lifestyle and how easily you can integrate monitoring into your daily routine.
- Technological Savvy: CGMs require more technical expertise than SMBG.
- Cost: CGMs are generally more expensive than SMBG systems. Insurance coverage for these devices varies.
Benefits and Considerations of SMBG
Benefits:
- Widely available and relatively inexpensive.
- Easy to use and portable.
- Provides immediate blood sugar readings.
Considerations:
- Requires finger pricking, which can be uncomfortable.
- Provides only a snapshot of blood sugar at a specific point in time.
Benefits and Considerations of CGM
Benefits:
- Provides continuous glucose readings, offering a more comprehensive picture of blood sugar trends.
- Can alert you to potential hypoglycemia or hyperglycemia events.
- Can help identify patterns missed with traditional finger pricking.
Considerations:
- Requires sensor insertion under the skin, which may be uncomfortable for some.
- More expensive than SMBG.
- May require calibration with finger pricking periodically.
- Technology dependence.
Interpreting Your Blood Sugar Readings
Each monitoring system will have its own target blood sugar range. However, here’s a general guideline:
- Before Meals: 80-130 mg/dL
- Two Hours After Meals: Less than 180 mg/dL
Taking Action Based on Your Readings
- High Blood Sugar (Hyperglycemia): If your blood sugar is consistently above target, consult your doctor to discuss potential medication adjustments, dietary changes, or increased physical activity.
- Low Blood Sugar (Hypoglycemia): If your blood sugar is below 70 mg/dL, consume a quick-acting source of sugar (glucose tablets, juice) and retest your blood sugar in 15 minutes.
Tips for Effective Blood Sugar Monitoring
- Monitor Regularly: Follow your doctor’s recommended monitoring frequency.
- Keep a Log: Record your blood sugar readings, along with information about meals, medications, and exercise, to identify patterns.
- Use Proper Technique: Ensure proper finger-pricking technique and device calibration for accurate readings.
- Cleanliness is Key: Wash your hands thoroughly before testing to prevent infection.
- Rotate Finger Prick Sites: Don’t prick the same fingertip repeatedly to avoid calluses.
- Travel Considerations: Pack enough supplies for your trip and discuss monitoring adjustments with your doctor if traveling across time zones.
- Discrete Monitoring: Discreet testing options are available for those who prefer privacy.
- Support System: Discuss your monitoring challenges with your healthcare team and seek their support.
Living with Blood Sugar Monitoring
- Blood sugar monitoring may seem like an additional burden, but with a positive attitude and proper integration into your routine, it can become a powerful tool for managing your diabetes. Here are some strategies for making monitoring a seamless part of your life:
- Set Realistic Goals: Start with a manageable monitoring frequency and gradually increase as needed.
- Find a Routine: Integrate monitoring into your daily routine, like before meals or before bed.
- Simplify the Process: Utilize tools like reminder apps or carrying cases to stay organized.
- Focus on the Benefits: Remind yourself of the positive impact monitoring has on your health.
Blood Sugar Monitoring and Technology
- Technology advancements offer exciting tools for diabetes management:
- Smart Glucometers: These connect to smartphones or computers, allowing for data storage, trend analysis, and sharing with healthcare providers.
- Continuous Glucose Monitoring (CGM) Apps: CGM systems often come with mobile apps that display real-time glucose trends, set alerts for high or low blood sugar, and integrate with insulin pumps for automated insulin delivery.
- Data Sharing Platforms: Secure platforms allow sharing your blood sugar data with your doctor or diabetes educator for remote monitoring and support.
The Future of Blood Sugar Monitoring
- The future of blood sugar monitoring is promising, with potential advancements like:
- Non-invasive Monitoring: Technologies that eliminate finger pricking altogether, like continuous glucose monitoring through sweat or interstitial fluid sensors.
- Artificial Intelligence Integration: AI-powered systems using your blood sugar data to predict trends and recommend personalized adjustments to diet, exercise, or medication.
- Closed-Loop Systems: Artificial pancreas systems that automatically adjust insulin delivery based on real-time glucose readings.
Conclusion
- Blood sugar monitoring is a crucial tool for anyone living with diabetes. By understanding the different monitoring systems, interpreting your readings, and taking action based on the results, you can actively participate in managing your diabetes and achieve optimal health. Embrace technology advancements and work with your healthcare team to create a personalized monitoring plan that empowers you to live a full and active life with diabetes.

 Diabetology2 weeks ago
Diabetology2 weeks ago
 Diabetology2 weeks ago
Diabetology2 weeks ago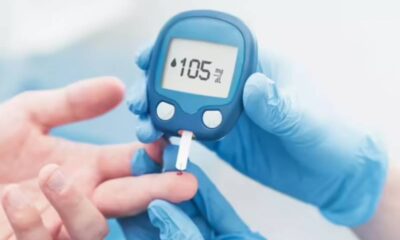
 Diabetology1 week ago
Diabetology1 week ago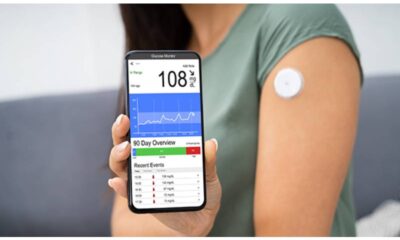
 Diabetology2 days ago
Diabetology2 days ago











