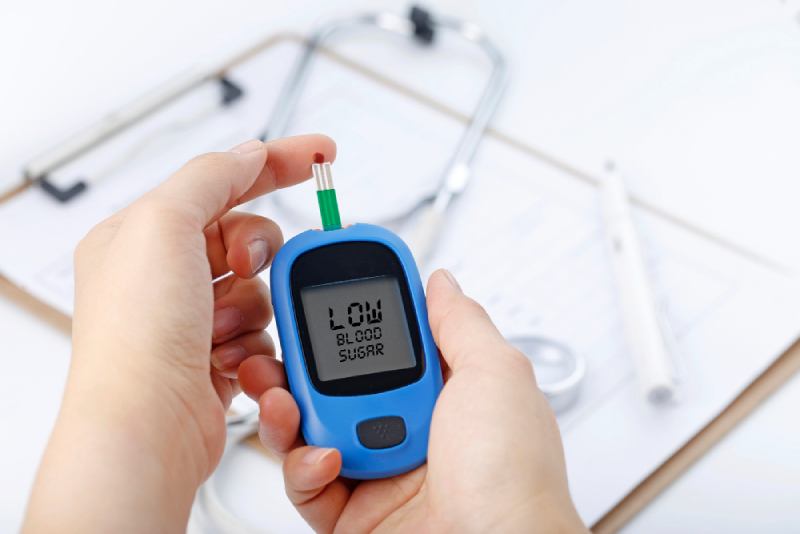
Diabetes mellitus, often simply referred to as diabetes, is a chronic health condition that affects how your body regulates blood sugar (glucose). This guide will equip you with a deep understanding of diabetes, including its types, causes, symptoms, diagnosis, treatment plans, management strategies, and potential complications.
Understanding Blood Sugar and Insulin
Blood sugar is the primary source of energy for your body’s cells. After you eat, your digestive system breaks down carbohydrates into glucose, which enters your bloodstream. The pancreas, a gland located behind your stomach, produces insulin, a hormone that acts like a key, unlocking the cells and allowing glucose to enter for energy use.
Types of Diabetes
There are three main types of diabetes:
- Type 1 Diabetes (T1D): An autoimmune disease where the body’s immune system attacks the insulin-producing cells in the pancreas. This leads to a complete or near-complete deficiency of insulin. T1D typically manifests in childhood or young adulthood and requires lifelong insulin therapy.
- Type 2 Diabetes (T2D): The most common form, accounting for around 90% of diabetes cases. In T2D, the body either develops insulin resistance (cells become less responsive to insulin) or has insufficient insulin production. T2D often develops in adulthood, but its prevalence is rising among children and adolescents. Management primarily focuses on lifestyle modifications, with medications or insulin potentially added when needed.
- Gestational Diabetes (GD): A temporary form of diabetes that develops during pregnancy. GD usually disappears after childbirth, but women with GD have a higher risk of developing type 2 diabetes later in life.
Risk Factors for Diabetes
While genetics play a role, several factors can increase your risk of developing diabetes:
- Family history: Having a parent or sibling with diabetes significantly increases your risk.
- Weight: Being overweight or obese is a major risk factor, especially for T2D.
- Physical inactivity: Regular exercise helps improve insulin sensitivity.
- Unhealthy diet: A diet high in processed foods, sugary drinks, and unhealthy fats can contribute to diabetes.
- Race/ethnicity: Certain ethnicities have a higher predisposition to T2D.
- Age: The risk of T2D increases with age.
- Polycystic ovary syndrome (PCOS) in women: This hormonal imbalance can increase diabetes risk.
Symptoms of Diabetes
Common symptoms of diabetes can include:
- Increased thirst and urination: The body tries to expel excess sugar through urine, leading to frequent urination and increased thirst to replenish fluids.
- Excessive hunger: Cells deprived of glucose due to insulin deficiency may signal hunger pangs.
- Unexplained weight loss: The body may break down muscle and fat for energy when glucose isn’t readily available.
- Fatigue and low energy: Cells not receiving enough glucose can lead to tiredness.
- Blurred vision: High blood sugar can affect the lenses in your eyes, causing blurry vision.
- Slow-healing sores: Reduced blood flow and nerve damage can impair healing.
- Frequent infections: Diabetes weakens the immune system, making you more susceptible to infections.
Diagnosing Diabetes
Doctors diagnose diabetes through blood tests that measure:
- Fasting plasma glucose (FPG): Blood sugar level after not eating for at least 8 hours.
- Hemoglobin A1c (HbA1c): Indicates average blood sugar control over the past 2-3 months.
- Random plasma glucose (RPG): Blood sugar level taken at any time, often used with other tests for confirmation.
Treatment Plans for Diabetes
The specific treatment plan for diabetes depends on the type and severity of your condition. Here’s a general overview:
- Type 1 Diabetes: Requires lifelong insulin therapy delivered through injections, pumps, or continuous glucose monitoring (CGM) systems.
- Type 2 Diabetes: Management often starts with lifestyle modifications like diet, exercise, and weight management. Medications like oral medications or injectable medications may be added if needed.
- Gestational Diabetes: Dietary changes and exercise are the primary focus. If these aren’t sufficient, medication may be necessary.
Living with Diabetes
Here are key strategies for managing diabetes effectively:
- Diet: Focus on a balanced diet rich in fruits, vegetables, whole grains, and lean protein. Limit processed foods, sugary drinks, and unhealthy fats.
- Exercise: Regular physical activity improves insulin sensitivity and overall health. Aim for at least 150 minutes of moderate-intensity exercise per week.
- Blood Sugar Monitoring: Blood sugar monitoring is a crucial aspect of diabetes management, allowing you to track your glucose levels and make informed decisions about diet, exercise, and medications.
Living a Healthy Life with Diabetes
Diabetes requires ongoing management, but it doesn’t have to limit your life. By following your doctor’s recommendations, adopting healthy habits, and staying informed about your condition, you can live a full and active life. Here are some additional tips:
- Regular Doctor Visits: Schedule regular checkups with your doctor to monitor your blood sugar control, adjust medications if needed, and address any concerns.
- Diabetes Education: Attending diabetes education programs can empower you with knowledge and skills for effective self-management.
- Foot Care: Diabetes can increase your risk of foot problems. Inspect your feet daily for cuts, blisters, or swelling, and practice proper hygiene.
- Dental Care: Maintain good dental hygiene to prevent gum disease, which can be more severe in people with diabetes.
- Stress Management: Chronic stress can elevate blood sugar levels. Practice relaxation techniques like deep breathing, meditation, or yoga.
- Support System: Connect with a diabetes support group or online community to share experiences and gain encouragement from others managing the condition.
Complications of Diabetes
If left uncontrolled, diabetes can lead to serious health complications, including:
- Heart disease and stroke: High blood sugar can damage blood vessels and increase the risk of heart attack and stroke.
- Nerve damage (neuropathy): Can cause pain, numbness, tingling, or weakness, especially in the feet and legs.
- Kidney disease (nephropathy): High blood sugar can damage the kidneys, leading to kidney failure.
- Eye problems (retinopathy): Can cause vision problems, including blindness.
- Foot problems: Nerve damage and poor circulation can increase the risk of foot ulcers, infections, and even amputation.
Conclusion
Understanding diabetes, its types, causes, symptoms, and management strategies is crucial for optimal health. With proper care and lifestyle modifications, you can manage your diabetes effectively and enjoy a long and healthy life. Remember, knowledge is power. Don’t hesitate to ask your doctor or diabetes educator questions and actively participate in your diabetes care plan.
Note: This guide provides general information and should not be considered a substitute for professional medical advice. Always consult with your doctor for personalized recommendations regarding diabetes management.

 Diabetology2 weeks ago
Diabetology2 weeks ago
 Diabetology2 weeks ago
Diabetology2 weeks ago
 Diabetology1 week ago
Diabetology1 week ago
 Diabetology3 days ago
Diabetology3 days ago