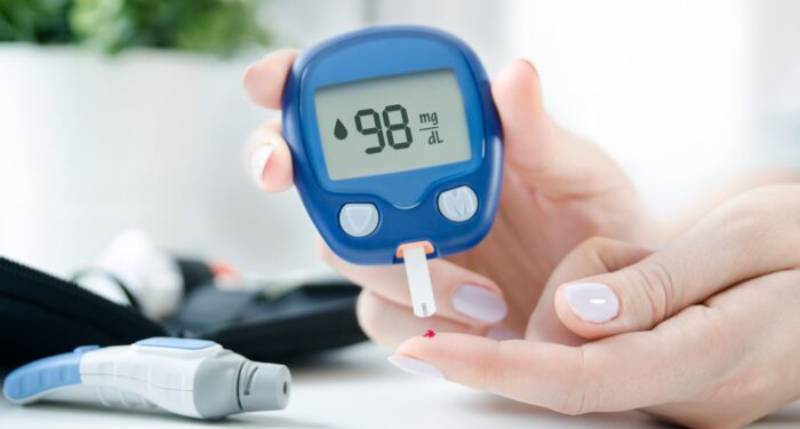
Insulin resistance is a fundamental concept in diabetes, yet it can be a complex topic to grasp. This comprehensive guide delves into the intricacies of insulin resistance, its impact on the body, and strategies for managing it.
What is Insulin Resistance?
- The Insulin-Glucose Connection: Insulin, a hormone produced by the pancreas, plays a crucial role in blood sugar regulation. It acts like a key, unlocking the doors to your body’s cells and allowing glucose (sugar) from your bloodstream to enter for energy production.
- Insulin Resistance Explained: In insulin resistance, these cellular “doors” become partially or completely blocked, hindering insulin’s ability to usher glucose into the cells. As a result, glucose builds up in the bloodstream, leading to hyperglycemia (high blood sugar).
Causes and Risk Factors for Insulin Resistance:
- Lifestyle Factors: Certain lifestyle choices significantly contribute to insulin resistance. These include:
- Obesity and Excess Belly Fat: Excess body fat, particularly around the abdomen, is a major risk factor. Fat cells can secrete substances that impair insulin sensitivity.
- Physical Inactivity: Regular physical activity enhances the body’s ability to utilize glucose effectively, improving insulin sensitivity.
- Unhealthy Diet: A diet high in processed foods, sugary drinks, and unhealthy fats can promote insulin resistance. Opt for whole grains, fruits, vegetables, and lean protein sources.
- Genetic Predisposition: Genetics play a role in insulin resistance susceptibility. If you have a family history of type 2 diabetes, your risk is higher.
- Other Factors: Certain medical conditions and medications can also contribute to insulin resistance, such as polycystic ovary syndrome (PCOS), Cushing’s syndrome, and some medications like steroids.
Consequences of Insulin Resistance:
- Prediabetes: Chronic insulin resistance can lead to prediabetes, a state where blood sugar levels are higher than normal but not high enough for a type 2 diabetes diagnosis.
- Type 2 Diabetes: Over time, the pancreas can struggle to keep up with the increased demand for insulin in insulin resistance, leading to the development of type 2 diabetes.
- Increased Risk of Other Health Problems: Insulin resistance is also linked to an increased risk of other health problems, including:
- Cardiovascular Disease: High blood sugar levels can damage blood vessels and increase the risk of heart attack, stroke, and peripheral artery disease.
- Fatty Liver Disease: Insulin resistance can contribute to the accumulation of fat in the liver, leading to nonalcoholic fatty liver disease (NAFLD).
- Metabolic Syndrome: This cluster of conditions includes high blood pressure, unhealthy cholesterol levels, and insulin resistance, significantly increasing the risk of cardiovascular disease and type 2 diabetes.
Diagnosing Insulin Resistance:
- Blood Tests: Several blood tests can assess insulin resistance, including fasting blood sugar, hemoglobin A1c (HbA1c), and oral glucose tolerance test (OGTT). However, these tests don’t directly measure insulin resistance. Doctors often rely on a combination of tests and clinical signs to make a diagnosis.
Strategies for Managing Insulin Resistance:
- Lifestyle Modifications: Fortunately, there’s good news! Lifestyle changes can significantly improve insulin sensitivity and reduce your risk of developing diabetes and other complications.
- Healthy Eating: Focus on a balanced diet rich in whole grains, fruits, vegetables, and lean protein. Limit processed foods, sugary drinks, and unhealthy fats.
- Regular Exercise: Aim for at least 150 minutes of moderate-intensity exercise or 75 minutes of vigorous-intensity exercise per week. Any physical activity is better than none.
- Weight Management: If you’re overweight or obese, losing even a modest amount of weight (5-10% of body weight) can significantly improve insulin sensitivity.
- Medications: In some cases, your doctor may prescribe medications to help manage blood sugar levels and improve insulin sensitivity. These may include metformin, a medication commonly used for type 2 diabetes management.
Living with Insulin Resistance:
- Monitoring Blood Sugar: Regularly monitor your blood sugar levels according to your doctor’s recommendations. This allows you to track progress and make adjustments to your management plan as needed.
- Maintaining a Healthy Lifestyle: Make healthy living a priority. Stick to a balanced diet, prioritize regular exercise, and get enough sleep.
- Partnering with Your Doctor: Maintain regular appointments with your doctor to discuss your progress, address any concerns, and adjust your management plan as needed.
- Building a Support System: Connect with support groups or online communities for people with insulin resistance or prediabetes. Sharing experiences, tips, and challenges can be incredibly motivating and provide valuable emotional support.
The Future of Insulin Resistance Research:
- Ongoing research is exploring new avenues for treating and potentially reversing insulin resistance. Some promising areas include:
- Novel Medications: Research is underway to develop new medications that target specific pathways involved in insulin resistance.
- Lifestyle Interventions: Studies are examining the potential of interventions like specific dietary patterns or exercise programs to improve insulin sensitivity more effectively.
- Precision Medicine: Researchers are exploring personalized approaches to managing insulin resistance, taking into account individual genetic and metabolic factors.
Conclusion:
Understanding insulin resistance empowers you to take control of your health and reduce your risk of developing diabetes and other chronic health conditions. By focusing on a healthy lifestyle, including a balanced diet, regular exercise, and weight management, you can significantly improve your insulin sensitivity and promote overall well-being. Remember, early intervention and ongoing management are key.
Disclaimer:
This information is intended for educational purposes only and should not be construed as medical advice. Always consult with your healthcare professional for personalized guidance on managing insulin resistance.
 Diabetology2 weeks ago
Diabetology2 weeks ago
 Diabetology7 days ago
Diabetology7 days ago
 Diabetology7 days ago
Diabetology7 days ago
 Diabetology4 days ago
Diabetology4 days ago
 Diabetology15 hours ago
Diabetology15 hours ago