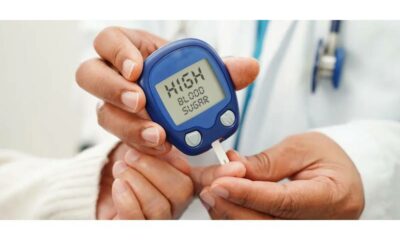
For people living with diabetes, maintaining healthy blood sugar levels is paramount. This not only helps manage symptoms but also reduces the risk of long-term complications. Regular blood sugar testing empowers you to take an active role in your diabetes management and make informed decisions about diet, exercise, and medication.
This comprehensive guide dives deep into the importance of regular blood sugar testing for diabetics, exploring its benefits, different testing methods, and how to interpret the results.
Why Blood Sugar Testing Matters:
Blood sugar, also known as glucose, is the primary source of energy for your body’s cells. When you eat, your body breaks down carbohydrates into glucose, which enters your bloodstream. The hormone insulin helps transport glucose into your cells for energy use.
In diabetes, the body either doesn’t produce enough insulin (type 1 diabetes) or can’t use insulin effectively (type 2 diabetes). This leads to chronically high blood sugar levels, which can damage nerves, blood vessels, and organs over time.
Regular blood sugar testing provides valuable insights into your body’s response to food, exercise, and medication. This information allows you to:
- Monitor Blood Sugar Control: Track how well your current diabetes management plan is working in keeping your blood sugar levels within target range.
- Identify Trends: Notice patterns in your blood sugar fluctuations, helping you adjust your diet, exercise, or medication accordingly.
- Prevent Complications: Early detection of high or low blood sugar levels allows for prompt action to prevent serious health problems.
- Make Informed Decisions: Empower yourself to make informed choices about your daily routine and diabetes management based on real-time data.
- Optimize Treatment: Assist your doctor in adjusting your medication dosage or treatment plan to achieve optimal blood sugar control.
Different Blood Sugar Testing Methods:
There are several methods for measuring blood sugar levels, each with its own advantages and limitations. Here’s a breakdown of the most common options:
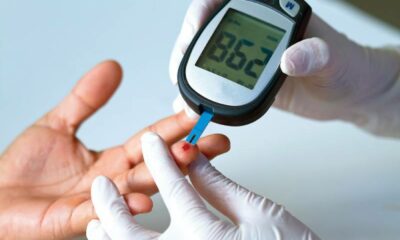
- Finger Prick Test (Blood Glucose Meter): This is the most widely used method. A small lancet pricks the fingertip, and a blood drop is placed on a test strip inserted into a blood glucose meter. The meter displays the blood sugar level in seconds.
- Continuous Glucose Monitoring (CGM): A small sensor is inserted under the skin, usually on the abdomen, to measure blood sugar levels continuously throughout the day and night. The sensor transmits data wirelessly to a receiver or smartphone app, providing real-time glucose readings and trends.
- Flash Glucose Monitoring (FGM): Similar to CGM, a sensor is inserted under the skin, but it doesn’t transmit data continuously. Instead, you scan the sensor with a reader to get a current blood sugar reading and some trend information.
Understanding Your Blood Sugar Results:
Blood sugar levels are typically measured in milligrams per deciliter (mg/dL). The American Diabetes Association (ADA) recommends the following target blood sugar ranges for most adults with diabetes:
- Before meals: 80-130 mg/dL
- Two hours after meals: less than 180 mg/dL
However, these are general guidelines. Your doctor will determine your specific target blood sugar range based on your individual health factors, type of diabetes, and overall treatment goals.
Interpreting your blood sugar results involves considering the timing of your test, recent food intake, and activity level. Here’s a breakdown of what your results might indicate:
- Below Target Range (Hypoglycemia): Symptoms may include sweating, shakiness, dizziness, and confusion. If your blood sugar falls below 70 mg/dL, consume quick-acting carbohydrates like fruit juice or glucose tablets.
- Within Target Range: This indicates good blood sugar control.
- Above Target Range (Hyperglycemia): Symptoms may include increased thirst, frequent urination, and fatigue. If your blood sugar remains consistently high, consult your doctor to adjust your medication or treatment plan.
Developing a Blood Sugar Testing Plan:
The frequency of blood sugar testing depends on various factors, including your type of diabetes, treatment plan, and overall blood sugar control. Your doctor will recommend a personalized testing schedule. Here’s a general overview:
- Type 1 Diabetes: Typically requires more frequent testing, often before meals, before bed, and sometimes at night.
- Type 2 Diabetes: Testing frequency can vary depending on treatment plan and blood sugar control. It might involve testing before meals, after meals, and before bed.
- Gestational Diabetes: Testing is usually done first thing in the morning and one or two hours after meals.
Conclusion:
Regular blood sugar testing is a cornerstone of effective diabetes management. By monitoring your blood sugar levels and understanding the results, you gain valuable insights into your body’s response to various factors. This empowers you to make informed decisions about your diet, exercise, and medication, ultimately leading to better blood sugar control and a healthier life. Remember, you are not alone in managing your diabetes. Work closely with your doctor, diabetes educator, and support system to create a personalized plan that works best for you.
 Diabetology2 weeks ago
Diabetology2 weeks ago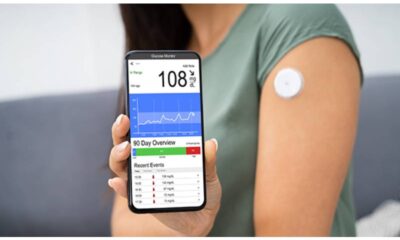
 Diabetology5 days ago
Diabetology5 days ago
 Diabetology1 day ago
Diabetology1 day ago
 Diabetology1 day ago
Diabetology1 day ago