Type 1 diabetes (T1D) is an autoimmune condition where the body attacks insulin-producing cells in the pancreas. This disrupts the body’s ability to regulate blood sugar (glucose) levels, leading to a variety of symptoms and potential health complications. While there’s no cure for T1D, effective management strategies can empower you to live a long, healthy, and fulfilling life.
This guide delves into the essential aspects of managing T1D, equipping you with knowledge and practical tools. We’ll explore:
- Understanding T1D: Causes, Symptoms, and Diagnosis
- Building a Strong Care Team
- Insulin Therapy: Types, Delivery Methods, and Adjustments
- Blood Sugar Monitoring: Importance and Techniques
- Carbohydrate Counting and Meal Planning
- Exercise and Physical Activity for Optimal Health
- Managing Stress and Emotional Wellbeing
- Preventing and Recognizing Complications
- Technological Advancements and Resources
- Living a Fulfilling Life with T1D: Travel, Relationships, and More
Understanding Type 1 Diabetes
Causes: T1D develops when the immune system mistakenly targets and destroys the insulin-producing beta cells in the pancreas. The exact cause remains unclear, but a combination of genetic predisposition and environmental factors likely plays a role.
Symptoms: Common symptoms of T1D include frequent urination, excessive thirst, increased hunger, unexplained weight loss, fatigue, blurry vision, and slow-healing wounds.
Diagnosis: Diagnosis typically involves a combination of blood tests, including a fasting blood sugar test, an A1C test, and an oral glucose tolerance test.
Building a Strong Care Team
A knowledgeable and supportive healthcare team is crucial for effective T1D management. This team often includes:
- Endocrinologist: A specialist in hormonal disorders, who will oversee your overall treatment plan and make medication adjustments.
- Diabetes Educator: This healthcare professional provides education and support on managing blood sugar, insulin therapy, nutrition, and lifestyle modifications.
- Dietitian: A registered dietitian can help you create a personalized meal plan to manage your blood sugar levels and maintain a healthy weight.
- Mental Health Professional: T1D can impact emotional well-being. A therapist or counselor can offer support for managing stress, anxiety, and depression.
Insulin Therapy: The Lifeblood of Management
Insulin is a hormone that helps your body absorb glucose from the bloodstream into your cells for energy. Since your body doesn’t produce enough insulin in T1D, managing blood sugar relies on external insulin administration.
Types of Insulin:
- Rapid-acting insulin: Starts working quickly (within 15 minutes) and peaks within 1-3 hours, ideal for covering meals.
- Short-acting insulin: Onset of action is within 30 minutes, peaking in 1-3 hours, and can be used for snacks or to correct high blood sugar.
- Long-acting insulin: Provides a continuous, low dose of insulin over a long period (up to 24 hours), used as a background to maintain stable blood sugar levels throughout the day.
Insulin Delivery Methods:
- Multiple Daily Injections (MDI): Injections are delivered subcutaneously (under the skin) using syringes or pens. Several injections may be required throughout the day, depending on insulin type and meal plan.
- Continuous Subcutaneous Insulin Infusion (CSII): An insulin pump delivers small, continuous doses of fast-acting insulin throughout the day. You can program the pump to adjust basal rates and boluses for meals and snacks.
Insulin Adjustments:
Your insulin needs can fluctuate due to factors like food intake, activity level, stress, and illness. Working with your doctor and diabetes educator is crucial to learn how to adjust your insulin doses based on these factors.
Blood Sugar Monitoring: The Key to Control
Regular blood sugar monitoring is essential for understanding how your body responds to food, insulin, and exercise. It allows you to make adjustments to your insulin regimen and avoid blood sugar swings.
Monitoring Techniques:
- Blood Glucose Meters: These portable devices require a finger prick to obtain a blood sample and measure your blood sugar level.
- Continuous Glucose Monitoring (CGM): These sensors are inserted under the skin and provide continuous readings of your blood sugar levels throughout the day, transmitted to a receiver or smartphone app.
Carbohydrate Counting and Meal Planning
Carbohydrates (carbs) are broken down into glucose in the body. Understanding how carbs affect your blood sugar is crucial for effective T1D management.
Carbohydrate Counting: This involves estimating the amount of carbohydrates in your meals and snacks to determine the appropriate insulin dose. It helps predict blood sugar spikes and maintain control.
Meal Planning:
Creating a personalized meal plan that incorporates your preferences, nutritional needs, and insulin regimen is essential. Here are some tips:
- Focus on whole foods: Prioritize fruits, vegetables, whole grains, lean protein, and healthy fats.
- Balance your plate: Include carbohydrates, protein, and healthy fats in every meal to ensure sustained energy and blood sugar control.
- Portion control: Use measuring cups and tools to ensure consistent portion sizes.
- Fiber is your friend: Fiber slows down the digestion of carbohydrates, helping to maintain stable blood sugar levels.
- Plan for snacks: Include healthy snacks throughout the day to prevent blood sugar dips.
- Read food labels: Pay attention to carbohydrate content and serving sizes.
Exercise and Physical Activity for Optimal Health
Regular physical activity offers numerous benefits for people with T1D, including:
- Improved blood sugar control
- Increased insulin sensitivity
- Weight management
- Reduced risk of cardiovascular disease
- Improved overall health and well-being
Managing Exercise:
- Consult your doctor before starting a new exercise program.
- Monitor your blood sugar levels before, during, and after exercise.
- Adjust insulin doses based on activity level.
- Stay hydrated before, during, and after exercise.
- Be prepared for blood sugar drops and carry fast-acting carbohydrates for correction.
Managing Stress and Emotional Wellbeing
Living with T1D can be stressful, and stress can in turn elevate blood sugar levels. Here are strategies for managing stress:
- Identify your stress triggers.
- Practice relaxation techniques like deep breathing, meditation, or yoga.
- Maintain a regular sleep schedule.
- Connect with supportive friends and family.
- Seek professional help if needed.
Preventing and Recognizing Complications
While T1D is a lifelong condition, effective management can minimize the risk of complications. These include:
- Diabetic retinopathy: Eye damage caused by high blood sugar levels.
- Diabetic neuropathy: Nerve damage that can cause pain, numbness, and weakness.
- Diabetic nephropathy: Kidney damage that can lead to kidney failure.
- Cardiovascular disease: Increased risk of heart attack and stroke.
Prevention Strategies:
- Maintain good blood sugar control.
- Manage blood pressure and cholesterol levels.
- Follow a healthy diet.
- Exercise regularly.
- Schedule regular check-ups with your healthcare team.
Recognizing Complications:
- Vision changes.
- Pain, numbness, or tingling in the hands and feet.
- Frequent urination or changes in urination patterns.
- Swelling in the feet or ankles.
- Unexplained fatigue.
Technological Advancements and Resources
Technology is constantly evolving to improve T1D management. Here are some advancements:
- Continuous Glucose Monitoring (CGM): Provides real-time blood sugar data and can be integrated with insulin pumps for automated adjustments.
- Insulin Pumps: Advanced pumps offer features like bolus calculators and closed-loop systems for automated insulin delivery.
- Diabetes Management Apps: These apps help track blood sugar, insulin doses, food intake, and exercise.
Living a Fulfilling Life with T1D
T1D doesn’t have to limit your life experiences. Here are some tips:
- Travel: Plan ahead for insulin supplies, blood sugar monitoring, and potential time zone changes.
- Relationships: Communicate openly with your partner or loved ones about your T1D needs.
- Education and Work: Talk to your school or employer about your T1D and advocate for necessary accommodations.
Conclusion
Thriving with T1D requires knowledge, commitment, and a supportive healthcare team. By implementing the strategies outlined in this guide, you can take control of your health, live a fulfilling life, and achieve optimal well-being. Remember, you are not alone. Utilize online resources, support groups, and educational programs to connect with others on the same journey. With dedication and a positive mindset, you can manage your T1D effectively and live a vibrant life.

 Diabetology2 weeks ago
Diabetology2 weeks ago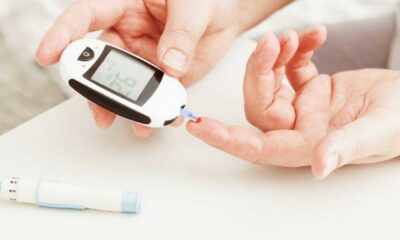
 Diabetology2 weeks ago
Diabetology2 weeks ago
 Diabetology1 week ago
Diabetology1 week ago
 Diabetology1 week ago
Diabetology1 week ago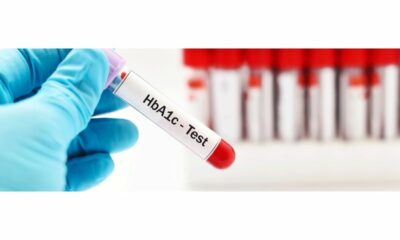
 Diabetology1 week ago
Diabetology1 week ago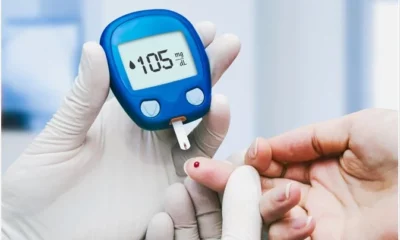
 Diabetology2 weeks ago
Diabetology2 weeks ago
 Diabetology1 week ago
Diabetology1 week ago
 Diabetology2 weeks ago
Diabetology2 weeks ago








